Six months after Eric Tennant died after a long battle with his health insurance company over doctor-recommended cancer treatment, West Virginia’s Republican governor signed a bill aimed at limiting the damage caused by insurance denials.
Subscribe to read this story without ads
Get unlimited access to ad-free articles and exclusive content.
Tennant, a coal mine safety instructor in Bridgeport, died last September at age 58 from complications related to stage 4 bile duct cancer. In early 2025, his insurance company, the State Public Employees Insurance Agency, repeatedly denied coverage for a $50,000 non-invasive cancer treatment that uses ultrasound to potentially target and shrink the largest tumors in his liver. His family didn’t expect the surgery to eradicate the cancer, but they hoped it would buy him more time and improve his quality of life. The insurance company said the procedure, called histotripsy, was not medically necessary and was considered “experimental and research.”
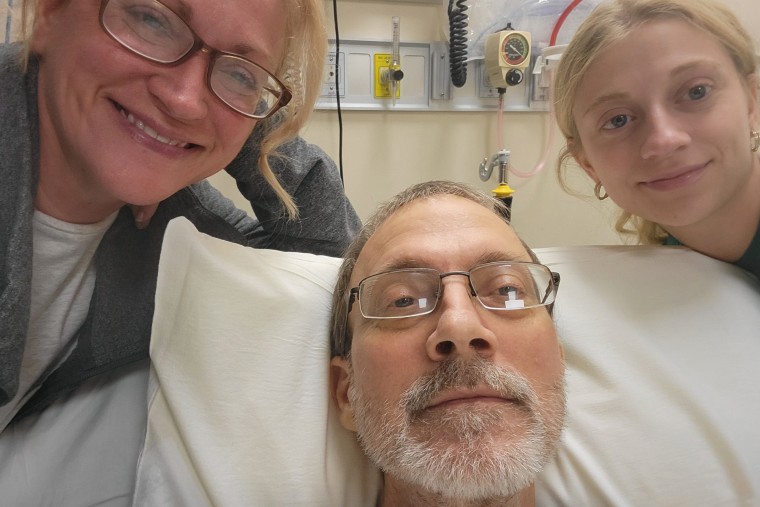
His widow, Becky Tennant, told West Virginia House committee members in late February that she had submitted medical records, expert opinions and data as part of several appeals of the denials. She also contacted “almost every state legislator” asking for help.
Nothing worked, she told lawmakers, until KFF Health News and NBC News got involved and questioned the Public Employees Insurance Agency about her husband’s case. Only then did the insurance company reverse its decision and approve tissue destruction, Tennant said.
“But by then, the delays had already taken their toll,” she said.
Within a week of the reversal in late May, Eric Tennant was hospitalized. His health continued to deteriorate, and by mid-summer he was no longer considered a suitable candidate for surgery. “The insurance company’s decision didn’t just delay treatment; it closed the door,” the wife said.
The West Virginia Public Employees Insurance Agency serves approximately 215,000 people, including state employees, their spouses, and dependents. The new law, which goes into effect on June 10, will allow plan participants who have been approved for a course of treatment to pursue a medically appropriate alternative treatment of equal or lesser value without requiring separate approval from a state-based health plan.

“This legislation is based on a simple principle: If a treatment is already approved, patients should be able to pursue medically appropriate alternatives without being forced to start the process over again, especially if they are less costly,” Gov. Patrick Morrissey said in a statement.
“This is about common sense, compassion and trusting patients and their doctors to make the best decisions for their care,” he said.
If the bill had gone into effect last year, Tennant could have undergone tissue removal without prior approval, said Republican Rep. Laura Kimble of Harrison, who introduced the bill. Because it was a cheaper alternative to chemotherapy that was already approved by insurance companies.
From Arizona to Rhode Island, at least half of all state legislatures this year have taken up bills related to prior authorization, the process by which patients and their medical teams must obtain insurance company approval before proceeding with treatment. The state efforts come as patients across the country wait for prior authorization hurdles to be eased, as promised by dozens of major health insurers in a pledge the Trump administration announced last year.
The West Virginia bill passed unanimously in the state Legislature and was signed by Morrisey on Tuesday. Kimble told KFF Health News the measure provides a “rational solution” for patients facing “the most irrational and chaotic time of their lives.”

U.S. health insurance companies claim that most prior authorization applications are approved quickly, if not immediately. AHIP, the health insurance industry trade group, says prior authorization serves as an important guardrail in preventing potential harm to patients and reducing unnecessary health care costs. However, studies have shown that denials and delays tend to affect patients who require expensive and time-sensitive treatments.
A poll released in February by the health information nonprofit KFF, which includes KFF Health News, found that Americans believe prior authorization is the biggest burden when seeking medical care.
Samantha Knapp, a spokeswoman for the West Virginia Department of Government, declined to answer questions about the law’s impact on the state’s finances. “At this time, we want to avoid any speculation regarding potential impacts or actions,” Knapp said.
Jason Haught, chief financial officer of the Public Employees Insurance Agency, said in a financial report attached to the bill that the legislation would cost the agency an estimated $13 million a year and “cause confusion for our members.”
In addition to the District of Columbia and Puerto Rico, West Virginia and 48 other states had already enacted some form of preclearance law or multiple such laws by late 2025, according to a report released in December by the National Association of Insurance Commissioners.
Many states have “gold card” programs that allow physicians with a proven track record of approval to bypass prior approval requirements. Some states have a maximum number of days that an insurance company can honor your request, while other states prohibit insurance companies from retroactively denying services after they are pre-approved. There are also a number of new state laws that seek to regulate the use of artificial intelligence in preauthorization decision-making.

Meanwhile, preclearance bills introduced this year across the country, including in Kentucky, Missouri and New Jersey, have support from politicians of both parties.
“Republicans in conservative states see health care as a vulnerability in the midterm elections, so naturally they’re going to do something about it,” said Robert Hartwig, a clinical associate professor of risk management, insurance and finance at the University of South Carolina. “They understand that they can’t do much at the federal level given the level of gridlock we’re already seeing.”
Last summer, the Trump administration released a pledge signed by dozens of health insurance companies pledging to reform prior authorization. Insurers promised to reduce the scope of claims that require pre-authorization, reduce wait times and communicate with patients in clear terms when denying claims.
Consumers, patient advocates and health care providers have expressed skepticism about whether companies will keep their promises.
Becky Tennant is also skeptical. That’s why she supported West Virginia’s bill.
“Families shouldn’t have to beg, plead, or go public just to receive time-sensitive care,” she told lawmakers. Tennant said she considers the bill’s passage bittersweet, but she thinks her husband would have been proud.
During Eric Tennant’s last hospital stay, just before she was discharged to home hospice care, she recalled asking her if she wanted to continue fighting to change the state’s prior authorization process.
“‘Well, you’ve got to at least try to change that,'” she recalled telling her husband. “Because it’s not fair.”
“I told him I would keep trying. At least for a while. So I will keep my promise to him.”
#West #Virginia #moves #preapproval #man #dies #due #insurance #denial
